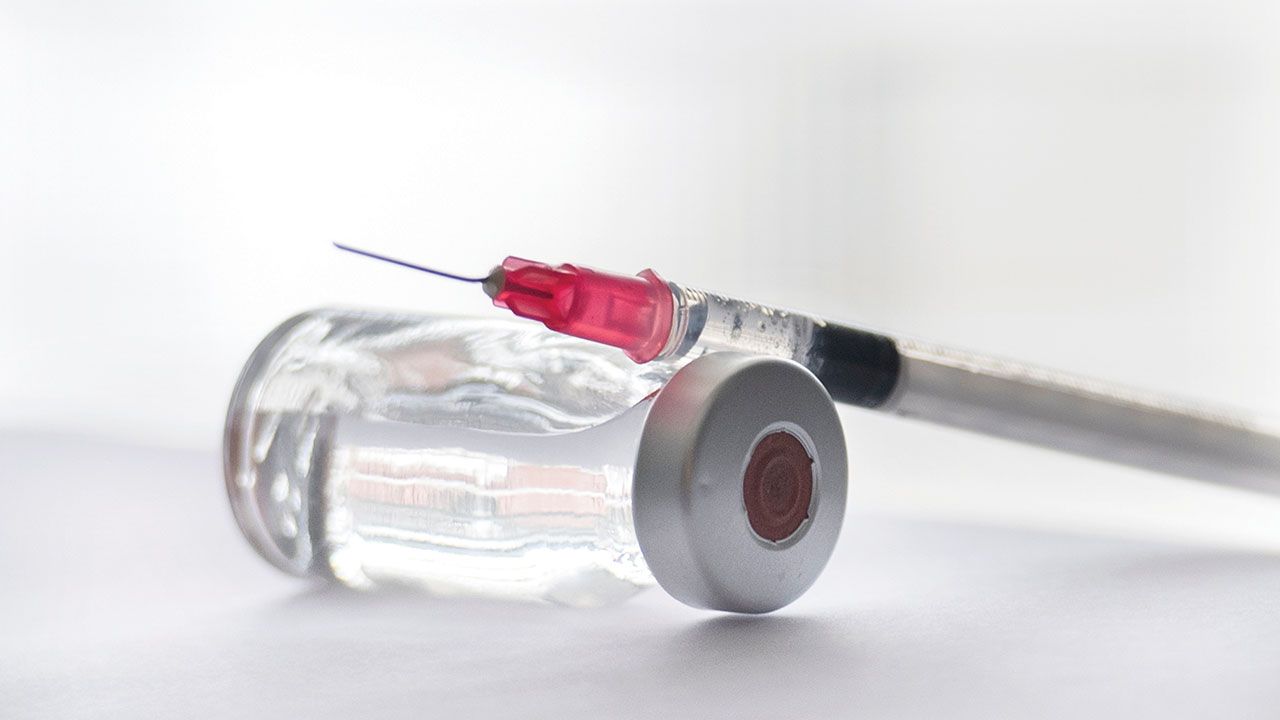
Manufacturing, Fill/Finish
Latest News
Latest Videos
More News

The European Commission’s approval of the Catalent acquisition by Novo Holdings includes the related acquisition of three manufacturing sites by Novo Nordisk, which is also acquiring the Czech Republic manufacturing site of Novavax for $200 million.

Cellipont Bioservices and Xiogenix Partner on Advanced Filling Systems The companies will offer Cellipont’s clients access to Xiogenix’ fill/finish system for cell therapy production.

With this $3.6 million investment, the CDMO will strengthen its advanced labeling, automated visual inspection, and fill/finish technology.

Aseptic fill/finish of biopharmaceuticals requires an understanding of the structure and limitations of each molecule.

The rising demand for biologics and technological innovations are driving blow-fill-seal capacity, harnessing manufacturing efficiency, and benefitting patients.

CDMO White Raven aims to reduce contamination risk and gain the capability to handle multiple product formats with the installation of Cytiva’s SA25 Aseptic Filling Workcell.

The Italian company’s North American business has seen an increase of 47%.

Given the criticality of fill/finish processes, it is clear that automation is the next technological step.

The partnership will allow for both companies to provide end-to-end biopharmaceutical manufacturing solutions.

The document includes recommendations for the reporting and implementation of changes to container closure system components.

Biosynth has further strengthened its peptide division with the acquisition of Pepceuticals.

With the acquisition, Sharp plans on offering fully integrated small-to-medium scale sterile injectable services.

Drug efficacy, reputation, and financial return are all on the line when it comes to fill/finish.

Kiefel’s new machine is designed to form, fill, and seal up to 6,000 infusion, parenteral nutrition, or dialysis bags per hour.
Use of a small-scale filler can result in increased filling efficiency.

This will allow industry leaders to make and sell the product, in addition to providing more choice to pharma and biotech companies.
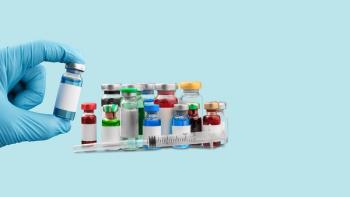
To prepare for emerging mRNA technologies, it is necessary to adapt fill/finish and cold chain capabilities.

Can CDMOs apply lessons learned from the COVID-19 pandemic to improve sterile processing?
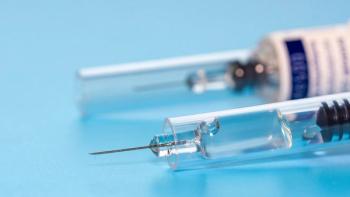
Shifts in pharmaceutical packaging have spurred tremendous growth in the pre-filled syringe fill/finish industry.

Steriline will be exhibiting its vial filling and capping machine (VFCM100) under double-wall isolator for aseptic filling at CPHI 2022 in Frankfurt, Germany, on Nov. 1–3, 2022.

Recipharm’s new high speed filling line, designed for pre-filled syringes and cartridges, is expected to be operational by May 2023.

Both demand for and investment in fill/finish capacity continue to rise.

BFS technology can help maintain sterility during the biologics manufacturing process.

Watson-Marlow and Franz Ziel GmbH have launched a new integrated solution to fast-track cell, gene, and biological therapies.

Grand River Aseptic Manufacturing has completed phase II of its facility expansion with the installation of two new sterile filling lines.